With the weather changing to summerly temperatures again, the incidence of thunderstorms and hence the incidence of lightning strikes will increase. Last month a group of 14 military cadets got injured by a lightning strike at the army base in Ossendrecht, the Netherlands. From a medical point of view, lightning is an interesting topic, with a lot of laymen’s myths that need to be adjusted. Fleetwood Mac’s “Dreams”-song which states that “thunder only happens when it rains”; not true! This brief review of the literature aims to provide relevant information for medical practice.
Lightning
Lightning is an electrical discharge caused by imbalances between storm clouds and the ground, or within the clouds themselves; most lightning occurs within the clouds. During a thunderstorm, an electrical gradient is formed by the interaction of moisture, warm air, and wind, and this current is eventually discharged as lightning. The exact science behind lightning has not been fully understood. However, a lot of hypotheses have been suggested (see this video).
Mechanism of injury
- Direct Strike: It is all in the name, the patient is hit directly by the bolt of lightning. It most commonly occurs to people who are caught in the open. Although it is relatively rare (5% of lightning strikes), it is, however, the deadliest type of hit.
- Side Flash (Side Splash): The lightning directly strikes an object such as a tree or building, but the current flow jumps (splashes) from its original pathway onto the victim (path of the lowest resistance). It is the most common cause of lightning injury. Splashes may occur from person to person when several people are standing close together. It accounts for 30% of all lightning strikes.
- Conduction (Contact Injury): Contact exposure occurs when a person is holding on to or touching an object that is either directly hit or splashed by lightning. The current passes through the object on to the victim. It occurs in 15% of lightning strikes.
- Ground Current (ground strike): Ground current is produced when lightning strikes the ground or a nearby object and the current spreads through the soil. If a person has one foot closer to the strike, then a potential difference may exist between the two feet (see this video), and the current will pass up one leg and down the other leg. This is a common mechanism for several people being injured at the same time (it accounts for 50% of all lightning strikes).
- Upward streamer injury: An electrical streamer heads upward into the sky but does not reach sky lightning and thus does not complete a connection. The electrical charge passes over and through the involved individual, but it is not nearly as powerful as that of a direct strike that comes from the sky.
See this link for more information about the different forms of a lightning strike.
Pathophysiology
Although the current flow occurs over a concise period (1/10.000; 1/1000 seconds), the amount of current is significant. Injuries occur from a “short-circuiting” of several of the body’s electrical systems as well as the more direct trauma and indirect trauma due to muscular contraction and being thrown.
Respiratory System: Acute respiratory arrest due to the loss of respiratory drive leading to life-threatening hypoxaemia. Pulmonary contusion and haemorrhage can also occur.
Cardiovascular: The most common cause of death in a lightning strike victim is a cardiac arrest. After the lightning strike, simultaneous depolarization of all the myocardial cells results in asystole or ventricular fibrillation and thus asystole. However, due to automaticity, the heart soon begins to contract in an organised manner. If a concomitant respiratory arrest occurs due to a paralysis of the medullary respiratory centre, the heart may deteriorate back into asystole secondary to the hypoxaemia. This respiratory arrest usually lasts longer than the cardiac arrest and is the major reason it is crucial to provide rescue breathing in lightning strike victims with cardiac arrest.
Other cardiovascular complications include direct myocardial damage or necrosis, coronary artery spasm, acute global cardiac dysfunction, atrial and ventricular dysrhythmias, pericardial effusion, ST-segment changes, as well as prolongation of the QT intervals.
Central Nervous System: When current traverses the brain, there can be coagulation necrosis of the brain, formation of epidural and subdural hematomas, intraventricular haemorrhage and paralysis of the respiratory centre. Patients who suffer cranial burns are four times more likely to die than those without cranial burns. Direct cellular damage to the respiratory and cardiac centres in the fourth ventricle of the brain may occur, especially if current passes through the orifices of the head. Seizures may occur secondary to the initial hypoxia from respiratory arrest or due to intracranial damage. These are usually transient, although they may continue for the first few days. Confusion and anterograde amnesia are very common.
Neuropsychological sequelae are very common: memory impairment, difficulty concentrating, sleep disturbances, personality change with increased lability and aggression.
Autonomic Nervous System (ANS): commonly, there is instability of the ANS for several hours after the injury. More severely injured patients may have lower extremity paralysis (keraunoparalysis) or in some cases, upper extremity paralysis
Peripheral Nervous System: paralysis, pain, and paresthesias. Symptoms may be delayed by weeks to years. If present, the prognosis is poor for recovery.
Skin consequences of a lightning strike: Deep burns are unusual after lightning injury. At most, some deep partial-thickness burns may occur. There are four types of skin effects:
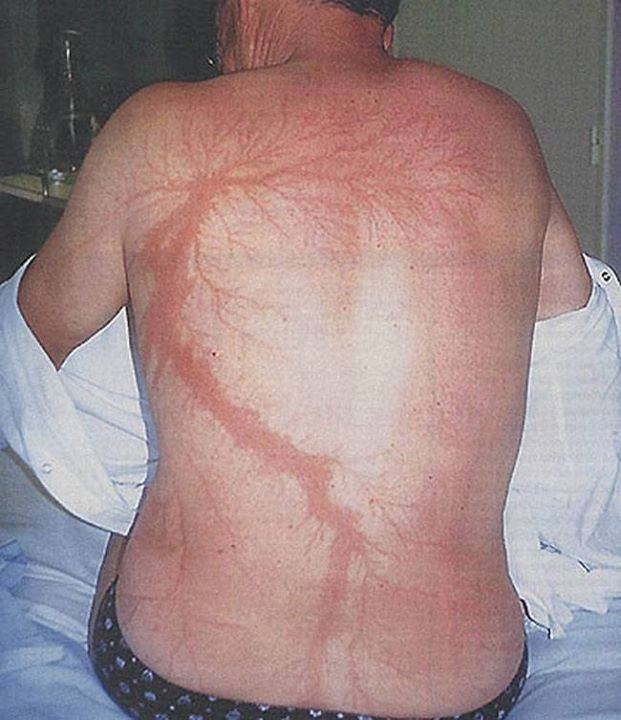
- Ferning (also called feathering or Lichtenberg figures: see FIGURE 1). These are not actual burns, but an unusual pattern that occurs due to the electron shower. This skin finding is pathognomonic for lightning injury.
- Linear burns: These are usually superficial and superficial-partial-thickness burns that occur from steam production from sweat or water on the victim due to the increased temperatures associated with the lightning strike.
- Punctate burns: These are multiple, closely spaced but discrete circular burns that individually range from a few millimetres to a centimetre in thickness. These resemble cigarette burns.
- Thermal burns: These are regular thermal burns that occur when a patient is wearing a metal object, such as a belt buckle or necklace, which heats up due to the electrical current travelling through it. There may also be thermal burns if clothing ignites.
Musculoskeletal System: Fractures and dislocations may occur due to intense muscular contraction or from being thrown. The significant muscular necrosis and extremity damage are seen in electrical injuries are unusual in lightning injuries.
In addition to flowing on the outside of the body (flashover), this current may also enter the body through the cranial orifices (eyes, ears, nose, and mouth) and flow through the body. This may explain why some patients have specific injuries such as ocular and ear, and others do not.
Ocular: One-half of all lightning victims will have ocular injuries. Cataracts are the most common ocular injury. These may develop immediately or as late as two years after being struck. Transient bilateral blindness of unknown aetiology is not uncommon. Dilated and unreactive pupils cannot be used as a sign of death, as this may occur after lightning injury.
Ear: Temporary deafness can occur due to the excessive noise and shock wave. 30 to 50 per cent of victims will sustain rupture to one or both tympanic membranes. Disruption of the ossicles and mastoid bone can occur. Also, facial palsies are seen, due to direct nerve damage of the facial nerve as it runs through the auditory canal.
Clinical presentation
The identification of a victim of a lightning strike is easy if the hit was witnessed. However, look for extra clues when the patient’s history is not that obvious. Suspect a lightning strike when the patient is confused, amnestic, dishevelled or possibly unconscious. Other hints that can assist you are environmental clues such as a recent storm or lightning. Physical findings such as fixed dilated pupils, ruptured tympanic membranes and the pathognomonic skin finding (Ferning sign) might help you diagnose the patient in case of an unwitnessed strike. The degree to which the patient demonstrates signs and symptoms of the lightning strike depends upon the type of strike they received (a direct hit causes the most severe symptoms).
The typical description of a multiple casualty lightning strikes is one of a sudden flash of bright light followed closely by a loud boom and then: chaos. There will likely be several people who are ambulatory but confused. There will be people who are lying on the ground but are at least moving or breathing on their own. These first two groups of people do not require immediate attention. The final group of casualties that do require your immediate attention is those who are unconscious, apnoeic, and pulseless; this approach is called reverse-triage.
The reason for this reverse triage is because those victims who are awake or at least breathing have survived the most immediate and potentially critical injury, which is a simultaneous cardiac and respiratory arrest. Those patients who are apnoeic and pulseless require Cardio-pulmonary-resuscitation (CPR) to get them to the point where their cardiac pacemakers restart, and their intrinsic respiratory drive has started again. These are the patients who may sustain cardio-respiratory arrest and regain their heartbeat but still require assistance with breathing for several minutes before their respiratory drive starts. In case of a real mass-causality situation: remember that patients with head burns are four times more likely to die from the strike!
First responder treatment
The first responder treatment should start with performing reverse triage and initiating CPR on those patients who are pulseless and apnoeic before caring for those who have spontaneous signs of life. Those with no spontaneous breathing or heartbeat may recover their heartbeat and will require assisted breathing until their respiratory drive returns. Breathing for these patients may prevent subsequent cardiac arrest due to hypoxia. If a victim does not regain a pulse within 20 to 30 minutes, then one may discontinue the resuscitation. Initial steps follow, as always, MARCH (CABC): massive haemorrhage, airway, respiration, circulation, and hypothermia/hyperthermia and hike versus hospital. Call for evacuation to the closest medical facility. Stabilisation such as splinting of fractures and spinal precautions should be performed as determined on your secondary assessment. The intra-hospital treatment of lightning strike victims depends strongly on the injuries sustained and is varies hence between every victim; the treatment is, however, supportive in intent.
Avoiding lightning injury
“When thunder roars go indoors”. If you hear thunder, then you should seek shelter. This is based on the fact that the distances that sound travels are well within the range of a lightning strike. Furthermore, you may miss lightning because the clouds or other terrain hides it: there is simply no safe place outdoors. Seek shelter in a substantial building or an all-metal vehicle. Small shelters such as golf, bus, and rain shelters may increase a person’s risk of being struck due to side splash as the lightning flows over the building (a so-called: “Faraday-Suit”). All metal vehicles are safe because the metal will diffuse the current around the occupants to the ground. It is a myth that rubber tires provide insulation.
If you are caught in a storm outside without a safe building or vehicle: Stay away from metal objects and those items that are taller than you. Avoid areas near power lines, pipelines, ski lifts, and other large steel objects. Do not stand near or under tall, isolated trees, hilltops, or at a lookout or other exposed area. In a forest, seek a low area undergrowth of saplings or small trees. Seek a clearing free of trees makes a person the tallest object in the clearing. If you are entirely in the open, stay far away from single trees to avoid lightning splashes and ground current. A good position is to squat down with your knees fully bent and your feet together or to sit cross-legged or to kneel on the ground (see FIGURE 2). Keeping the feet together prevents you from being injured by the ground current. If you are in a group of people, then spread far apart so that a single lightning strike will not take out the entire group. The group members should be separated by more than 20 feet (6 m) to limit the potential for mass casualties due to a strike and the ground current. This allows the individuals to watch others and to rescue them if struck. If you are on the water, seek the shore and avoid being the tallest object near a large body of water.

If indoors: Avoid open doors and windows, fireplaces and metal objects such as sinks and plugged-in electrical appliances. Do not talk on the telephone as telephone lines may not be grounded like electrical wires.
Also, see the recommendations regarding thunderstorms and lightning from the Dutch fire brigade (via this link), the tips are, however, in Dutch!
References:
- Life in the fast lane – Lightning strikes: https://bit.ly/2X3qlnl
- Davis, C., Engeln, A., Johnson, E. L., McIntosh, S. E., Zafren, K., Islas, A. A., … & Cushing, T. (2014). Wilderness Medical Society practice guidelines for the prevention and treatment of lightning injuries: 2014 update. Wilderness & environmental medicine, 25(4), S86-S95: https://bit.ly/2ZwqrR5
- Minute Earth – how to survive a lightning strike: https://bit.ly/2N3LCbO
- NOS article about the lightning strike during military training: https://bit.ly/2J0i35H
- National Geographic: The Science of Lightning: https://bit.ly/2gvJTLG
- Dutch fire brigade regarding thunderstorms and lightning: https://bit.ly/2vzIcD5
- FIGURE 1: Domart, Y., & Garet, E. (2000). Lichtenberg figures due to a lightning strike. New England Journal of Medicine, 343(21), 1536-1536.
- FIGURE 2: Davis, C., Engeln, A., Johnson, E. L., McIntosh, S. E., Zafren, K., Islas, A. A., … & Cushing, T. (2014). Wilderness Medical Society practice guidelines for the prevention and treatment of lightning injuries: 2014 update. Wilderness & environmental medicine, 25(4), S86-S95:



